The monkeypox virus (MPXV) can spread from animals to humans and between humans, causing the disease mpox. In recent years, MPXV has evolved into two distinct genetic groups, known as "clades". While clade I predominantly occurs in Central Africa, clade II of the MPXV was reported for the first time in over 100 countries worldwide, including Switzerland, in summer 2022. Moreover, since September 2023, the World Health Organization (WHO) reported an increase of a new MPXV sub-variant (clade Ib) in the Democratic Republic of Congo, which has recently spread to several neighboring countries. Consequently, in August 2024, the WHO declared this epidemic a "public health emergency of international concern". Although the symptoms of mpox are generally mild, often including flu-like symptoms and rash development, complications can occur. Between 1985 and 2021, approximately 3% of individuals infected with MPXV developed neurological symptoms such as seizures or encephalitis, with some cases being fatal. Yet, the extent to which the MPXV affects the human central nervous system remains poorly understood.
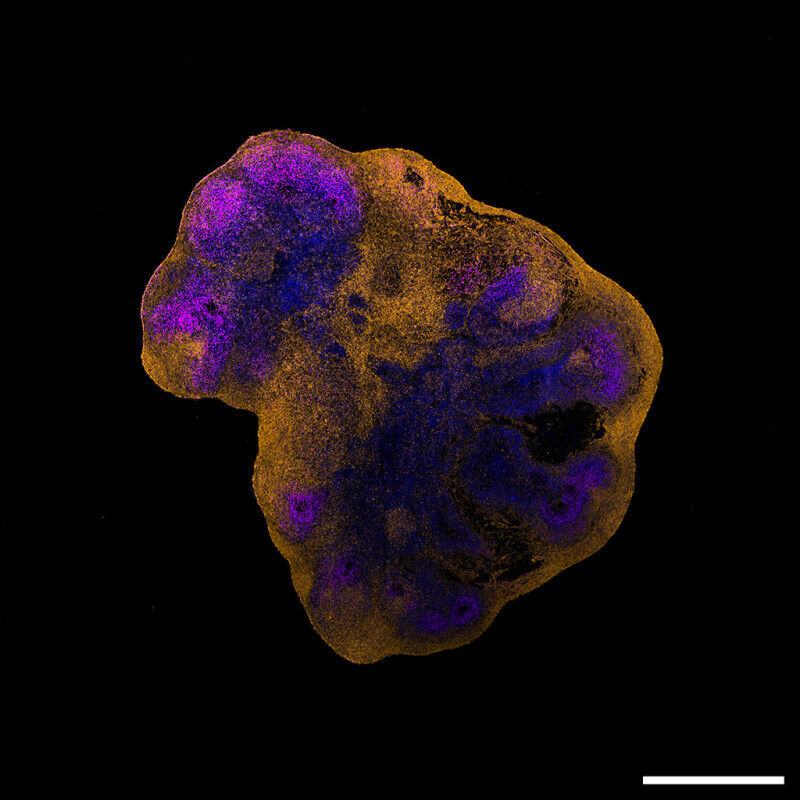
Brain organoids: a promising model for studying neurological disorders
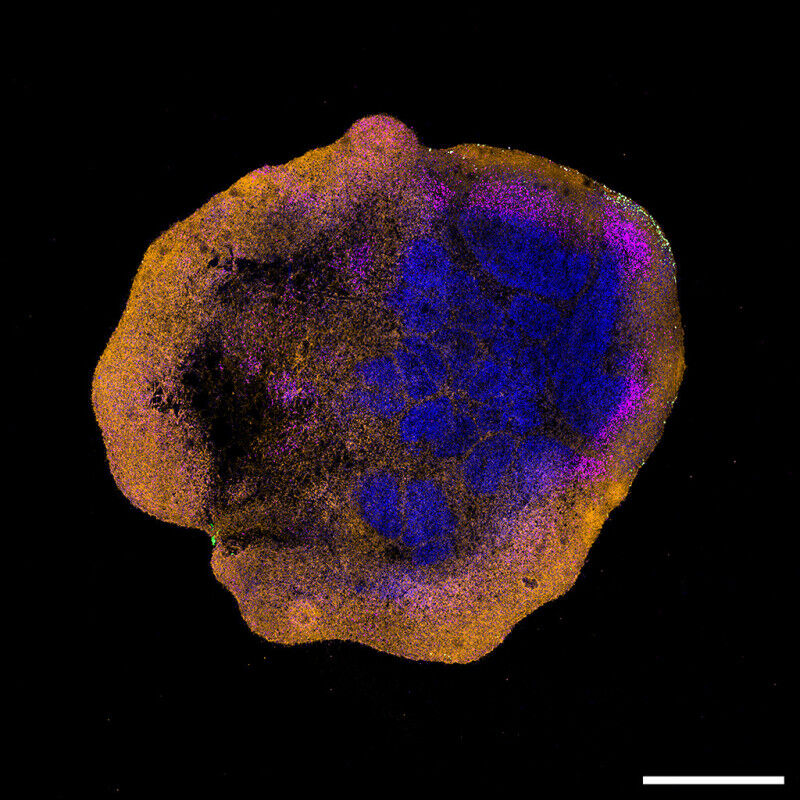
Prior to this study, neurological manifestations had already been reported in patients with MPXV infection. In animal studies, viral components were also detected in the brain of infected animals. However, the mechanisms underlying these neurological symptoms have remained largely unexplored. "This is likely because the virus was, for a long time, geographically restricted and there were few available samples and models to investigate its impact on the nervous system", says Marco Alves from the IVI and the University of Bern, last author of the study.The team of researchers used innovative human brain organoids to study how the MPXV spreads in the brain. "Brain organoids are 3D tissue models generated from human pluripotent stem cells. As they mature into neural tissue, they form structures that recapitulate specific brain features. Although complex to generate, brain organoids hold enormous potential for studying neurological diseases" explains Isabel Schultz-Pernice, PhD candidate at the IVI and the University of Bern and first author of the study. The cultivated organoids were then exposed to a virus sample isolated from a patient infected during the 2022 outbreak. "Using advanced imaging techniques, we were able to observe how MPXV spreads within these neuronal cells" she adds. "These experiments would have been extremely difficult, if not impossible, to conduct in vivo due to ethical and practical constraints. This underlines the strong potential of brain organoids as a human-relevant alternative to animal models", says Marco Alves.
MPXV causes neuronal cell death in organoids
Using their model, the researchers demonstrated that the virus spreads from cell-to-cell along neurites, the thin fibers that connect neurons. In the process, the MPXV manipulates the cells’ transport machinery, resulting in the formation of so-called "neuritic beads". These bead-like swellings are also a hallmark of neurodegenerative diseases such as Alzheimer’s. The formation of neuritic beads ultimately precedes neuronal cell death.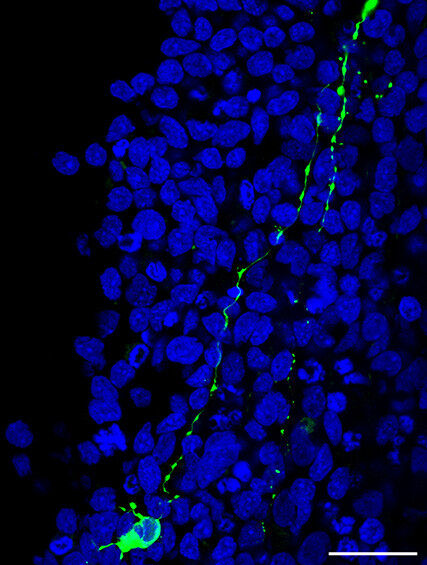
Innovative research under high security conditions
In light of the recent global rise of Mpox cases, these new findings are highly significant, not only for the fields of virology and neurobiology, but also from a public health perspective. The results highlight a previously unexplored aspect of MPXV infection, its neuropathological potential. They underscore the need for further research in this area, while also contributing to the development of targeted therapeutic strategies."The collaboration of researchers with extensive experience in handling high-risk pathogens, combined with state-of-the-art infrastructure, was crucial to the success of this study", concludes Alves.


