A UNIGE and HUG team has, for the first time, described the interaction between the cerebellum and the brain’s reward system in people with schizophrenia.
Schizophrenia is a neuropsychiatric disorder that affects around 1% of the population and is best known for its hallucinatory and delusional symptoms. However, it is also marked by profound apathy, a reduced ability to experience pleasure, and progressive social withdrawal. These so-called "negative" symptoms - for which no effective treatment currently exists - are particularly disabling.
We show that stronger cerebellar regulation of the reward system is associated with a reduction in negative symptoms - and conversely, weaker regulation with an increase in symptoms.
Several studies have shown that abnormalities in the brain’s reward system - particularly in the dopamine-producing ventral tegmental area (VTA) - are associated with these symptoms. In people with schizophrenia, the VTA is believed to be overactive, leading to a blunted perception of salience, where "everything feels the same," and resulting in a lack of motivation.
The cerebellum, a hidden regulator
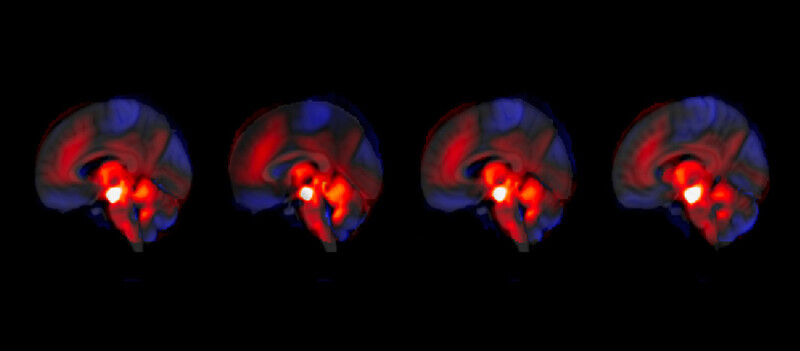
In an innovative study, a team from the University of Geneva and the Geneva University Hospitals (HUG) has shown that the cerebellum plays a key role in regulating - or dysregulating - this mechanism via the VTA. "What is sometimes called our ’little brain’ actually contains 50% of all’our neurons. Although it was long considered to have a purely motor function, we are now discovering that it also plays important emotional and cognitive roles," explains Indrit Bègue, assistant professor in the Laboratory of Neuroimaging and Translational Psychiatry in the Department of Psychiatry at the University of Geneva Faculty of Medicine, researcher at the Synapsy Centre for Neuroscience Research in Mental Health, and University hospital physician in the Department of Adult Psychiatry at HUG, who led the study.By following 146 patients over a period of 3 to 9 months, and by analysing an independent validation cohort, the team was able to observe and describe for the first time the functional connection between the cerebellum and the VTA in the context of schizophrenia. "We show that stronger cerebellar regulation of the reward system is associated with a reduction in negative symptoms - and conversely, weaker regulation with an increase in symptoms. This newly identified mechanism opens up promising avenues for targeted therapeutic interventions," explains Jade Awada, a doctoral candidate in Indrit Bègue’s team at the Laboratory of Neuroimaging and Translational Psychiatry in the Department of Psychiatry at the University of Geneva Faculty of Medicine, researcher at the Synapsy Centre for Neuroscience Research in Mental Health, and first author of the study. The analyses were carried out by Jade Awada and Farnaz Delavari, co-first author of the study and researcher in Professor Stephan Eliez’s laboratory.

